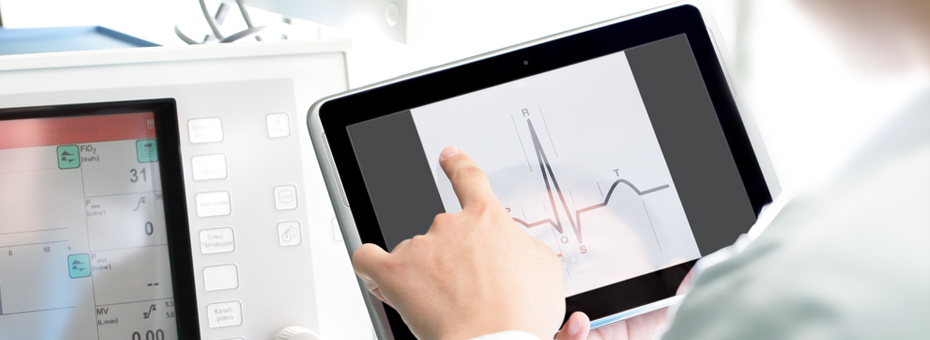
Healthcare technology, including HIT (Healthcare Information Technology) is improving healthcare delivery in many different ways. Telemedicine allows physicians to remotely diagnose and prescribe treatment for patients in rural areas and remotely monitor patients in understaffed critical care units. Pacemakers can now tell the wearer when his or her heart rate is too fast. Patient portals permit patients to schedule appointments, view their records, request prescription refills, and ask questions of their providers. Kiosks are speeding up the check in process at clinics and hospitals.
On the other hand, technology always adds cost and may even create more work for the staff members who must use it. For example, as we learned in his presentation at the MHA (Michigan Health and Hospital Association) Keystone Center’s Annual Symposium on Patient Safety and Quality in April, Dr. Peter Provonost of Johns Hopkins recently observed that his hospital had to add a nurse FTE in critical care because the hospital’s new EMR and its computerized heparin infusion pumps didn’t talk to each other. That meant one nurse had to manually enter orders from the EMR for each infusion pump administering heparin four times a day and a second nurse, according to hospital policy, observed the order entry to ensure there were no errors. Some primary care practices have concluded that their new electronic health records are no better than spreadsheets; they’re just more costly and less user friendly.
Some technology actually puts patients at risk. On Father’s Day, Parade Magazine carried a “Smart Move of the Week” about apps that purport to help users distinguish normal moles from those that are cancerous. However, a 2013 study in JAMA Dermatol indicated that three of the four apps in the study incorrectly identified 30 percent of melanomas as benign.
Technology should support the worker (and the patient), not vice versa. Jeffrey Liker speaks to this in chapter 14 of The Toyota Way, “Principle 8: Use Only Reliable, Thoroughly Tested Technology That Serves Your People and Processes.” The book Kaizen Express discusses this idea as well in the section, “Separating Human Work and Machine Work.” This will mean something different for each organization, but here are some possible implications for yours:
1) Work flows/processes should be designed to deliver safe and effective care in the most efficient manner possible and HIT should be modified to support those processes, not the other way around.
2) New technologies should be able to marry with existing technologies, not create workarounds for staff members who provide the linkage.
3) New technologies should provide genuine value to their users (providers and patients), not just novelty.
How do you see technology improving (or not improving) the work in your organization? What are you doing to make sure technology is being used well?